Get Healthy!
- Dennis Thompson
- Posted August 25, 2023
Sepsis Almost Killed Jake Tapper's Daughter, Alice. Now, She's Working to Keep Others Safe
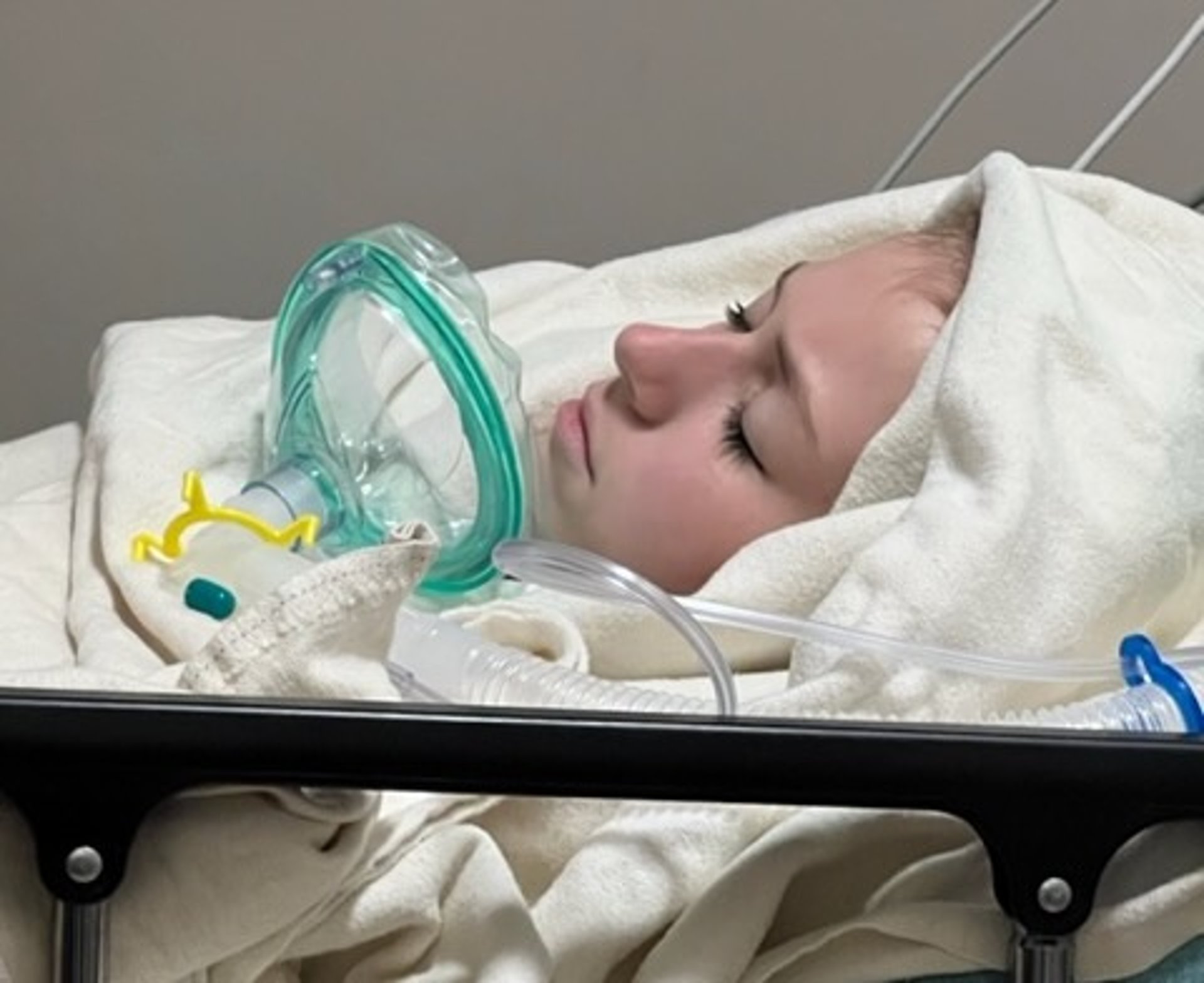
Alice Tapper felt deathly ill, suffering from severe abdominal pain, a 102-degree fever and vomiting.
Emergency room doctors found that Alice -- the daughter of CNN anchor Jake Tapper -- had a rapid pulse of 135 beats per minute and a very high white blood cell count, indicating her body was fighting off a severe infection.
The doctors gave her IV fluids "¦ and that was it.
"We were told this was a viral infection and that we essentially needed to wait it out," said Alice, now 15 and a high school junior in Washington, D.C. "My parents consulted with multiple doctors about what could be done and asked about possible treatments and more tests, but we were told that none were needed."
In fact, Alice had developed sepsis, a life-threatening condition in which a severe infection triggers a chain reaction in the body that can lead to organ failure.
Alice and her mother, Jennifer Tapper, spoke out Thursday during a U.S. Centers for Disease Control and Prevention media briefing aimed at raising public awareness of the risk of sepsis.
"My heart was breaking and I was losing my daughter and I couldn't get anyone to listen,"Jennifer Tapper recalled. "This was my reality one horrible Tuesday night in November 2021, and I never want anyone to go through what we had to go through.
"My husband Jake and I are so grateful that Alice survived, but we are also angry that her infection was missed and that she could have died as a result,"she added.
Parents and patients need to ask about the possibility of sepsis if a severe infection leads to hospitalization, the Tappers and CDC officials said during the briefing.
"If I could turn back the clock, my first words when we brought Alice to the hospital would have been, 'Is this sepsis?'" Jennifer Tapper said.
At the same time, doctors need to take concerns over sepsis seriously and be ready to respond, officials added.
Misdiagnosis, and finally, help
Sepsis contributes to at least 1.7 million adult hospitalizations and 350,000 deaths each year in the United States, according to a report on sepsis care in the CDC's latest Morbidity and Mortality Weekly Report.
Unfortunately, more than 1 U.S. hospital in 4 (27%) does not have a committee that monitors and reviews sepsis care, the report found.
Further, only 55% of hospitals with a sepsis committee set aside time for leaders to manage the program and conduct daily activities.
"I will say that as a physician who has cared for those patients, it requires rapid coordination between multiple hospital departments and disciplines to respond and then manage the recovery of the patient," CDC Director Dr. Mandy Cohen said at the briefing.
Any type of infection can cause sepsis, but most cases result from a bacterial infection, according to the CDC.
In Alice Tapper's case, it was a perforated appendix that was undiagnosed.
Over two days, her condition worsened, but her doctors maintained she just had a bad stomach virus.
"I was losing so much weight and could barely stay awake," Alice said. "Luckily, my dad was very persistent and determined. He found a health care professional who took additional steps. He made sure I got an X-ray. That led to a sonogram and surgery."
The CT scans showed fluid leaking throughout her abdomen.
"I was rushed to the ICU," Alice said. "I was septic and the appendix was too inflamed to be removed."
As a result of her sepsis, Alice also had developed hypovolemic shock, a condition in which a person has lost so much blood that organs can't get the oxygen and nutrients needed to function.
"My story ends on a positive note, but not before several additional surgical procedures, including getting my appendix out and a long procedure to repair my bowels," Alice said. "I fully recovered. I'm healthier and stronger than ever, and I've become a high school athlete."
A complex condition
"Now I'm on a mission to tell my story and encourage hospitals to listen to patients, even if they are young, and to parents," Alice said. "If appendicitis had been taken seriously and the signs and symptoms of sepsis had been acknowledged, my course of care would not have resulted in weeks in hospital and a long recovery at home."
The consequences have been profound.
"I missed so much school and so much of my life and I lost a lot of my trust in adults. Now I'm speaking up for others who do not have a voice," Alice concluded.
 Alice (l.) and Jennifer Tapper
Alice (l.) and Jennifer Tapper
The challenge is that sepsis can look very different from patient to patient, said Dr. Chris DeRienzo, chief physician executive for the American Hospital Association, who spoke at the briefing.
DeRienzo's specialty is neonatology, where "sometimes the only and earliest sign of sepsis in an extremely premature baby was a slight drop in heart rate."
In an elderly patient with heart failure, a warning sign for sepsis might be newly developed shortness of breath, DeRienzo said -- but "sometimes it can be really challenging to know whether that new shortness of breath is coming from worsening of their heart failure or as an early sign of sepsis."
Sepsis is a complex condition, he emphasized.
"Its early signs can often be masked when patients have multiple health issues," DeRienzo said. "It is essential to bring together experts from across the hospital in a multidisciplinary approach to build those programs targeted at early identification and treatment."
Dr. Hallie Prescott, who helped craft the CDC's Hospital Sepsis Program Core Elements, a guide to improving sepsis care, agreed that the condition is tricky to diagnose.
"One of the challenges is that sepsis can look very different across different people and can also kind of overlap with other types of conditions,"Prescott, an associate professor of pulmonary and critical care medicine at the University of Michigan, said at the CDC briefing.
"We wish we had one blood test or one diagnostic test that could just say, yes, this patient has sepsis or no, they don't, but we just don't have that," Prescott said. "So it does really require a holistic assessment of a patient's clinical presentation as well as their presenting testing."
Hospitals respond
The CDC's recommendations for hospitals emphasize the need to provide resources to a multi-disciplinary sepsis team, appoint a leader, put clinical guidelines in place, actively track sepsis cases, report these cases to public health officials, and make sure ongoing sepsis education is provided to health care professionals and patients.
Unfortunately, more than 1,400 hospitals around the nation have no sepsis program in place, the new report found.
"About 1,400 hospitals are basically starting from scratch,"said Dr. Raymund Dantes, a CDC medical adviser and co-developer of the Hospital Sepsis Program Core Elements. "They don't have a sepsis committee yet and we want to encourage them to go ahead and get started, and we provide that guide to get started."
The program is also geared to help hospitals where programs are already in place.
"For those hospitals that have already got sepsis programs underway and have available resources, we have a lot more details and best practices that we've collected from hospitals about how to further improve your sepsis program," Dantes said.
Jennifer Tapper presented a list of sepsis warning signs that parents should know, including:
- High heart rate
- Weak pulse
- Fever
- Shivering
- Cold hands or feet
- Confusion or disorientation
- Shortness of breath
- Extreme pain or discomfort
- Clammy and sweaty skin
She urged health care professionals to listen "to caregivers and parents and the patients, including teens, because they know what they're talking about."
More information
The U.S. Centers for Disease Control and Prevention has more about sepsis.
SOURCES: Mandy Cohen MD, MPH, director, U.S. Centers for Disease Control and Prevention, Atlanta; Chris DeRienzo, MD, chief physician executive, American Hospital Association, Chicago; Hallie Prescott, MD, MSc, associate professor, pulmonary and critical care medicine, University of Michigan, Ann Arbor; Raymund Dantes, MD, CDC medical adviser, Atlanta; Alice and Jennifer Tapper, Washington D.C.; Morbidity and Mortality Weekly Report, Aug. 25, 2023







